in this article
authors
Prostate cancer is one of the most common cancers in men worldwide. While treatments can be effective early on, advanced disease is often difficult to control. One of the key weapons in fighting cancer, immunotherapy, hasn’t been very effective in the prostate. Immunotherapy harnesses the body’s own immune cells to fight tumors. These sentinels roam the body through the bloodstream to keep you healthy, attacking pathogens, viruses, and malfunctioning cells that turn into cancer.

A new study in the journal Immunity reveals that the prostate has its own defense force and unlocks key insights into how this army of cells, known as tissue-resident memory CD8 T cells, or Trm cells, works.
“We found that different types of T cells live in different areas, or neighborhoods, within the tissue, and where they live determines how they behave,” said Kennidy Takehara, Ph.D., scientist at the Allen Institute and lead study author. “This is important because these long-lived immune cells can help recognize and fight cancer. By understanding what helps these cells survive and function, we may be able to design therapies that boost the body’s own immune response against prostate tumors.”
what did researchers discover about trm cells?
Researchers at the Allen Institute; University of California, San Diego Moores Cancer Center; and La Jolla Institute for Immunology discovered that Trm cells act differently depending on where they lived inside the prostate. Like real estate, location matters.
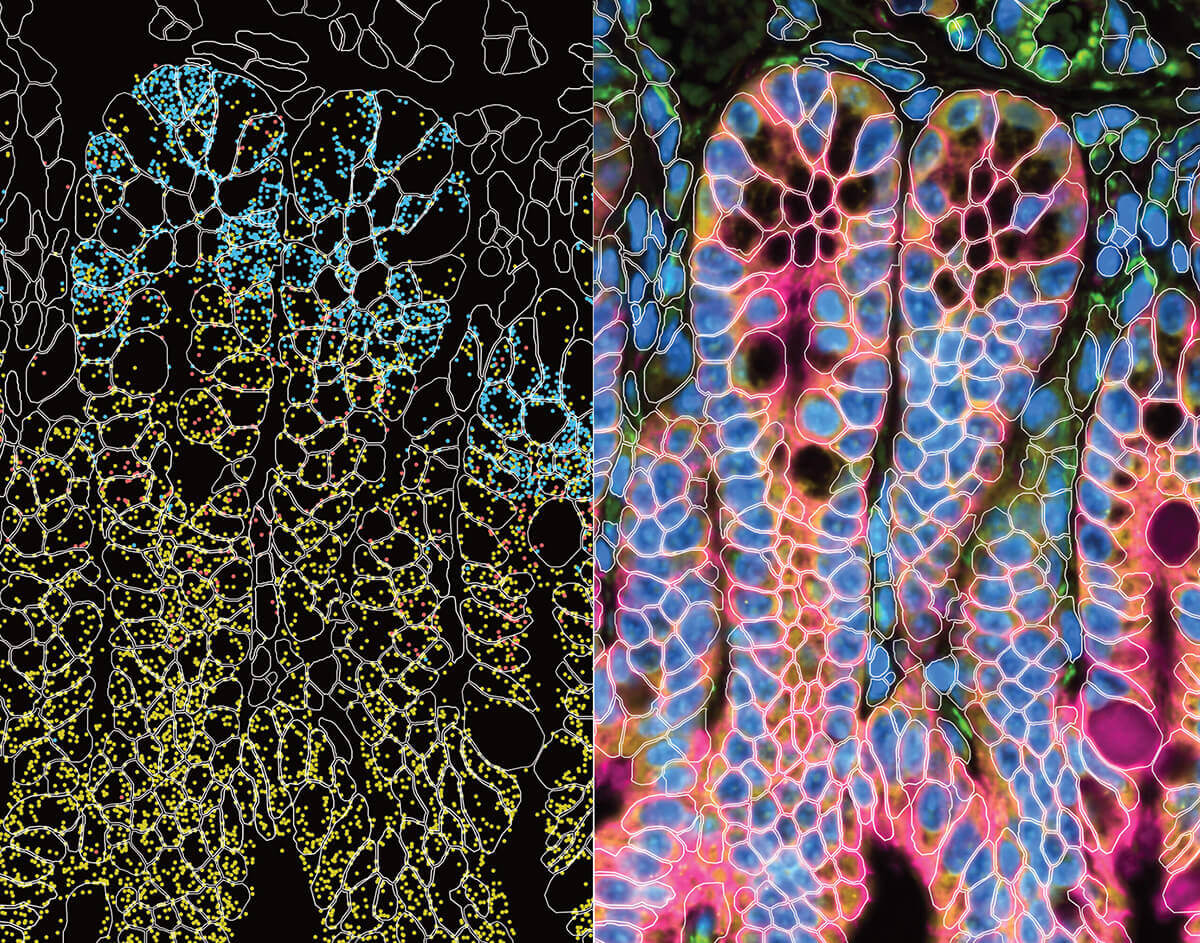
The prostate is made up of two distinct neighborhoods: the epithelial glands, where the organ’s primary work occurs, and the stroma, the connective tissue scaffold that holds everything together.
The Trm cells located near the glands were more cytotoxic and associated with active immune defense; in other words, they were the enforcers doing the fighting and killing cancerous cells and viruses.
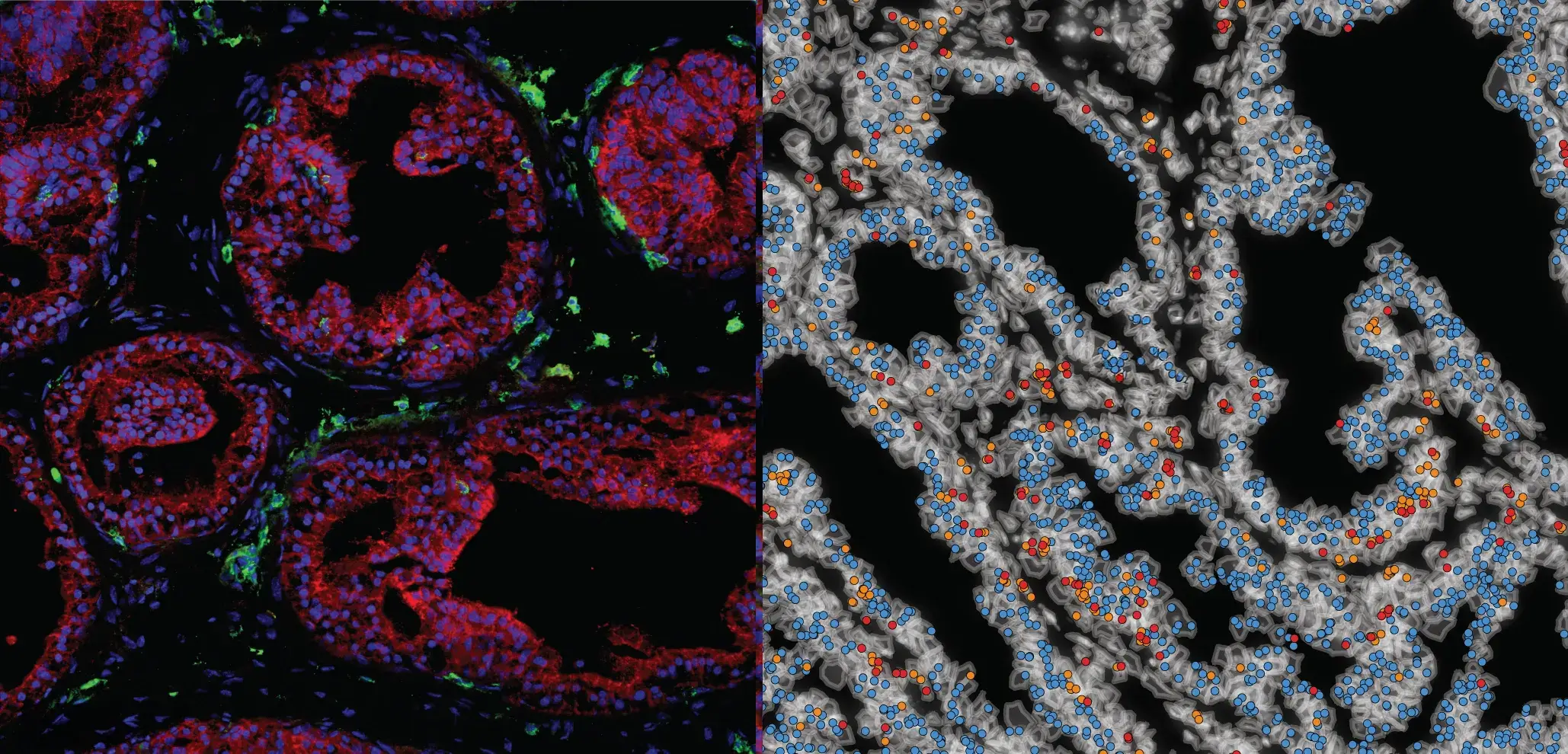
The Trm cells in the stromal regions played a more strategic and supportive role in immune defense. They were able to recognize, or “remember,” past infections or pathogens and trigger an immune response when the same invader was encountered again—even transforming into fighting immune cells that helped clear infection or cancer.
“This study provides a key framework for understanding prostate T cell immunity. Going forward, we are committed to understanding how to leverage these insights in the context of prostate cancer and cancer immunotherapies,” says Miguel Reina-Campos, Ph.D., co-senior author of the study and assistant professor at La Jolla Institute for Immunology.
why this matters for cancer immunotherapy
Why does immunotherapy work for some cancers but fail in the prostate? The answer may lie in “location, location, location.” Scientists discovered that T cells behave differently based on which prostate neighborhood they lived in. This means that in the future, researchers might be able to tailor treatments relative to where a tumor is located within the body, ensuring the immune cells are “tuned” to the right frequency to attack.

“We were really excited about the findings because we had observed in a previous study that location matters in the small intestine too. And we didn’t know if this was going to be a universal truth or if this was something very specific about the unique environment of the small intestine,” said Ananda Goldrath, Ph.D., scientific advisor at the Allen Institute, Presidential Chair in Molecular Biology at UC San Diego, and co-senior author of the study. “This does show that there are rules for how T cells are arranged in tissues and they are similar across tissues. By understanding these rules we can get a handle on in general impacting inflammation across tissues.”
By unlocking the secret life of T cells in the prostate, this research moves us one step closer to personalized medicine that could lead to more effective cancer treatments. Researchers can now look toward new therapies that activate and reprogram the defense force already stationed in the prostate. This approach could also be applied to cancer of other organs to develop tailored treatments and therapies that are both more effective and less harmful to the rest of the body.
Citations
about the allen institute
Allen Institute is a 501(c)(3) nonprofit medical research organization dedicated to accelerating science for a healthier world. Through large-scale, multidisciplinary research initiatives, the Institute generates foundational knowledge, data, tools, and models that are shared openly with the world to advance our understanding of life and health. Founded by Jody Allen and the late Paul G. Allen, Allen Institute is supported primarily by the Fund for Science and Technology.


.avif)